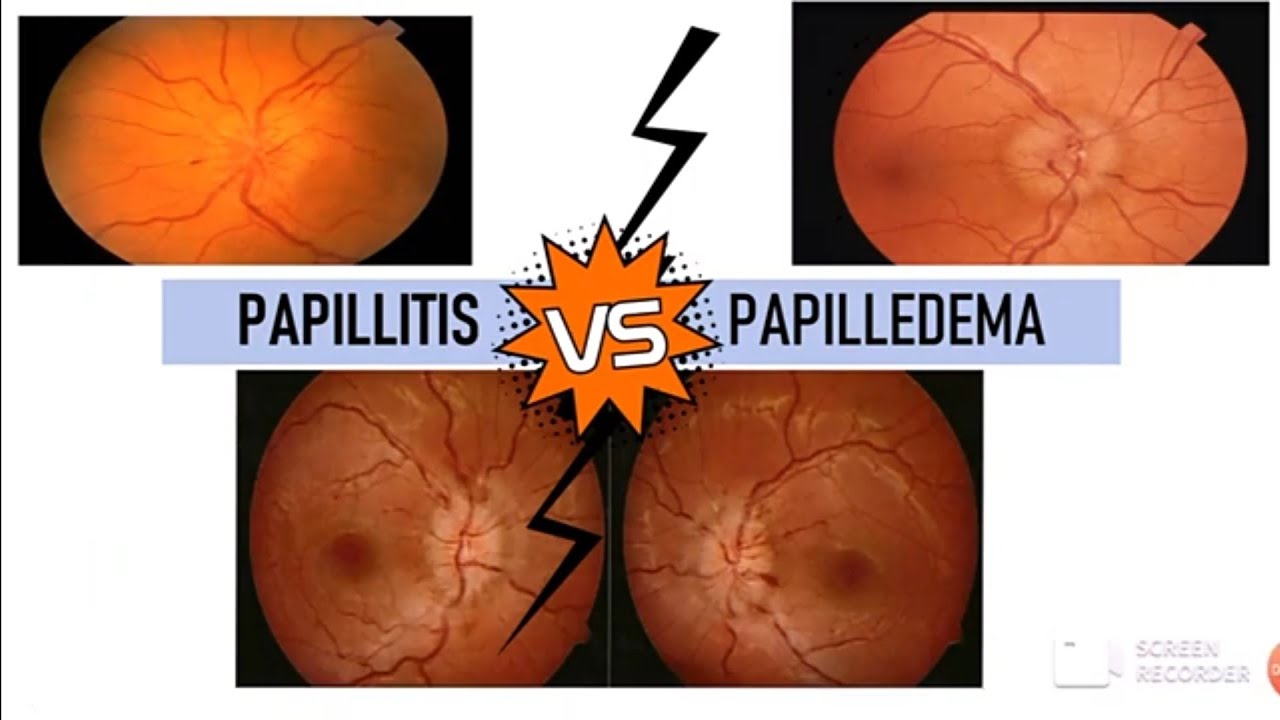
Differences Between Papillitis and Papilledema
Papillitis Vs Papilledema
Here is a detailed table comparing
Papillitis (Optic Neuritis) and
Papilledema:
.responsive-table {
width: 100%;
border-collapse: collapse;
margin: 20px 0;
font-size: 18px;
text-align: left;
}
.responsive-table th, .responsive-table td {
padding: 12px;
border: 1px solid #ddd;
}
.responsive-table th {
background-color: #4CAF50;
color: white;
text-align: center;
}
.responsive-table tbody tr:nth-child(even) {
background-color: #f2f2f2;
}
.responsive-table tbody tr:hover {
background-color: #ddd;
}
/* Responsive Design */
@media screen and (max-width: 768px) {
.responsive-table {
display: block;
overflow-x: auto;
white-space: nowrap;
}
}
| Feature | Papillitis (Optic Neuritis) | Papilledema |
|---|---|---|
| Usually Affects | Unilateral (U/L) | Bilateral (B/L) |
| Onset | Sudden | Insidious/Chronic |
| Loss of Vision | Marked, painful | Negligible, gradual |
| Pain with Eye Movement | Present | Absent |
| Tenderness | Present at the insertion of MR & SR | Absent |
| Other Symptoms | Usually not seen | Headache, nausea, vomiting (↑ ICP) |
| Swelling (Edema) of Disc | 2-3D swelling | >3D swelling, marked blind spot enlargement |
| Visual Field Defect | Centrocecal scotoma | Enlarged blind spot |
| Color Vision | Reduced (Dyschromatopsia) | Normal |
| Pupillary Reflex (RAPD) | Present (Positive) | Absent |
| Posterior Vitreous | Fine opacities present | Clear |
| Cause | Optic neuritis, Multiple sclerosis, infections | Increased intracranial pressure (tumor, hydrocephalus, meningitis) |
| Management | Steroids (IV Methylprednisolone) | Treat underlying cause (reduce ICP) |
 |
| Papillitis Vs Papilledema |
MCQs on Vision and Optic Pathology
-
What is the most common cause of papilledema?
a) Optic neuritis
b) Increased intracranial pressure
c) Glaucoma
d) Retinal detachment -
Which of the following is NOT a feature of papilledema?
a) Bilateral involvement
b) Enlarged blind spot
c) Sudden painful vision loss
d) Absence of RAPD -
A patient with optic neuritis is likely to have which of the following?
a) Unilateral sudden vision loss
b) Marked papilledema
c) Gradual vision loss
d) Normal pupillary reflexes -
The presence of a relative afferent pupillary defect (RAPD) suggests:
a) Glaucoma
b) Optic neuritis
c) Retinal detachment
d) Conjunctivitis -
What is the primary treatment for optic neuritis?
a) Acetazolamide
b) Intravenous steroids
c) Antibiotics
d) Antihypertensives -
Which condition is associated with a centrocecal scotoma?
a) Papilledema
b) Papillitis
c) Retinitis pigmentosa
d) Diabetic retinopathy -
Which of the following is NOT a common cause of increased intracranial pressure?
a) Brain tumor
b) Hydrocephalus
c) Optic neuritis
d) Meningitis -
What visual defect is classically seen in papilledema?
a) Central vision loss
b) Enlarged blind spot
c) Peripheral scotoma
d) Homonymous hemianopia -
A 25-year-old female with multiple sclerosis presents with unilateral painful vision loss. What is the most likely diagnosis?
a) Glaucoma
b) Papilledema
c) Papillitis (Optic neuritis)
d) Retinal detachment -
The presence of dyschromatopsia (impaired color vision) is most commonly associated with:
a) Papillitis
b) Papilledema
c) Cataract
d) Age-related macular degeneration
Answer Key:
- b
- c
- a
- b
- b
- b
- c
- b
- c
- a