Table of Contents
Video on Chron’s Disease (sensitizer)
🔬 Overview & Definition





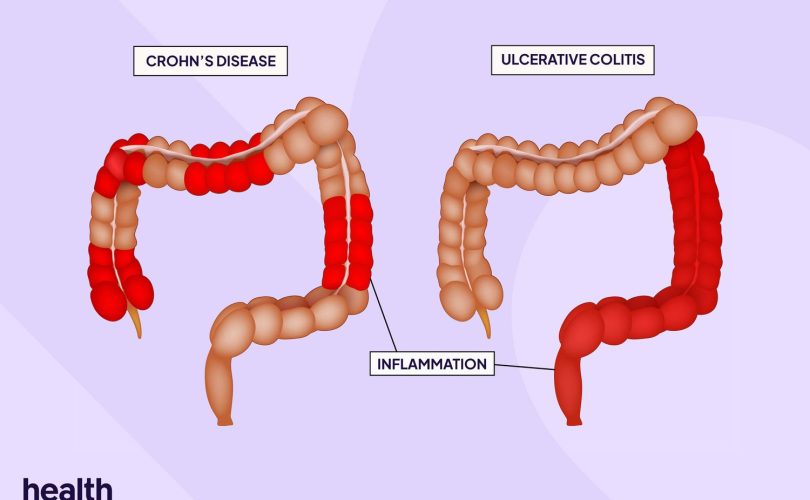
Crohn’s disease (CD) is a chronic, relapsing inflammatory bowel disease (IBD) characterized by:
- Transmural inflammation
- Segmental (“skip”) involvement
- Can affect any part of GI tract (mouth → anus), most commonly:
- Terminal ileum ± colon
🧬 Etiopathogenesis
1. Genetic Susceptibility
- Strong association with:
- NOD2 (CARD15) mutation
- Other genes: ATG16L1, IL23R
- Family clustering common
2. Immune Dysregulation
- Predominantly Th1 and Th17 mediated response
- ↑ Cytokines:
- TNF-α, IL-12, IL-23
- Impaired regulatory T-cell function
3. Microbiome Interaction
- Dysbiosis with abnormal response to gut flora
- Loss of tolerance to commensals
4. Environmental Factors
- Smoking (↑ risk, worse prognosis)
- NSAIDs, infections, diet
🧠 Pathology
Gross Features







- Skip lesions
- Cobblestone appearance
- Strictures (“string sign”)
- Creeping fat
Microscopy
- Transmural inflammation
- Non-caseating granulomas (not always present)
- Lymphoid aggregates
- Fissuring ulcers → fistula formation
📍 Distribution Patterns
- Ileocolonic (most common)
- Isolated ileal
- Isolated colonic
- Upper GI involvement (rare but important)
⚠️ Clinical Features
Intestinal Symptoms
- Chronic diarrhea (may be non-bloody)
- Abdominal pain (RLQ common)
- Weight loss, malnutrition
- Fever during flares
Complications
- Strictures → obstruction
- Fistulas:
- Enteroenteric
- Enterocutaneous
- Perianal (hallmark)
- Abscess formation
Extraintestinal Manifestations
- Joints: peripheral arthritis, ankylosing spondylitis
- Skin: erythema nodosum, pyoderma gangrenosum
- Eyes: uveitis, episcleritis
- Hepatobiliary: PSC (less common than in UC)
🔎 Diagnosis
1. Endoscopy (Gold Standard)
- Patchy inflammation
- Aphthous ulcers → deep linear ulcers
- Cobblestone mucosa
2. Imaging
- MR enterography preferred
- CT for complications
- Barium:
- String sign
3. Histology
- Transmural inflammation
- Granulomas (supportive, not mandatory)
4. Laboratory Findings
- ↑ CRP, ESR
- Anemia (iron deficiency, chronic disease)
- Hypoalbuminemia
- Fecal calprotectin ↑
🧾 Differential Diagnosis
- Ulcerative colitis
- Intestinal tuberculosis (important in Nepal)
- Infectious enterocolitis
- Ischemic colitis
🧑⚕️ Disease Classification
Montreal Classification
- Age at diagnosis (A1–A3)
- Location (L1–L4)
- Behavior:
- B1: inflammatory
- B2: stricturing
- B3: penetrating
💊 Management (Step-Up vs Top-Down Approach)
1. Induction Therapy
Mild–Moderate
- Budesonide (ileocecal disease)
- 5-ASA (limited role in CD)
Moderate–Severe
- Systemic corticosteroids
2. Maintenance Therapy
- Thiopurines (azathioprine, 6-MP)
- Methotrexate
- Biologics:
- Anti-TNF:
- Infliximab
- Adalimumab
- Anti-integrin:
- Vedolizumab
- Anti-IL-12/23:
- Ustekinumab
- Anti-TNF:
3. Surgical Management
- Not curative (unlike UC)
- Indications:
- Obstruction
- Fistula
- Abscess
- Refractory disease
🚨 Complications
- Short bowel syndrome
- Malabsorption (B12 deficiency)
- Colorectal cancer (less than UC but still increased risk)
- Osteoporosis (steroid use)
📊 Prognosis
- Chronic relapsing course
- Majority require surgery at some point
- Smoking cessation improves outcomes significantly
🧠 High-Yield Harrison Pearls
- Transmural + skip lesions = Crohn’s
- Perianal disease strongly suggests CD
- Granulomas: specific but not sensitive
- Surgery is not curative
- Anti-TNF revolutionized management