Table of Contents
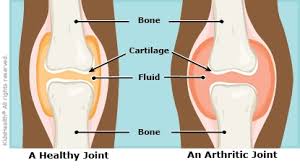
JIA = Juvenile Idiopathic Arthritis
A chronic inflammatory arthritis of unknown cause beginning before age 16 and lasting ≥ 6 weeks, after exclusion of other causes.
✅ Definition (Juvenile Idiopathic Arthritis)
- Arthritis in ≥1 joint
- Onset < 16 years
- Duration ≥ 6 weeks
- Other causes excluded (infection, malignancy, trauma, connective tissue diseases)

🧬 ILAR Classification (Most used worldwide)
1️⃣ Oligoarticular JIA
Most common type (~50%)
Criteria
- ≤4 joints involved in first 6 months
Subtypes
- Persistent: remains ≤4 joints
- Extended: becomes >4 joints after 6 months
Features
- Large joints (knee most common)
- Asymmetric
- ANA positive common
- Risk of uveitis
2️⃣ Polyarticular JIA (RF negative)
Criteria
- ≥5 joints in first 6 months
- RF negative
Features
- Small joints of hands/feet
- Symmetrical
- Chronic course
3️⃣ Polyarticular JIA (RF positive)
Criteria
- ≥5 joints
- RF positive (≥2 tests, 3 months apart)
Features
- Similar to adult rheumatoid arthritis
- Severe, erosive disease
- Adolescents (girls common)
4️⃣ Systemic JIA (Still disease)
Criteria
- Arthritis with or preceded by fever ≥2 weeks
- Daily (quotidian) fever for ≥3 days
PLUS ≥1: - Evanescent salmon-pink rash
- Hepatosplenomegaly
- Lymphadenopathy
- Serositis
Features
- High ferritin
- Risk of MAS (macrophage activation syndrome)
5️⃣ Enthesitis-related Arthritis (ERA)
Criteria
Arthritis + enthesitis
OR arthritis/enthesitis + ≥2:
- Sacroiliac tenderness/inflammatory back pain
- HLA-B27 positive
- Male >6 years
- Acute anterior uveitis
- Family history of spondyloarthropathy
Features
- Lower limb arthritis
- May progress to ankylosing spondylitis
6️⃣ Psoriatic Arthritis
Criteria
Arthritis + psoriasis
OR arthritis + ≥2:
- Dactylitis
- Nail pitting/onycholysis
- Psoriasis in first-degree relative
7️⃣ Undifferentiated JIA
- Does not fit above categories
OR fits more than one category
🧪 Diagnostic Criteria & Workup
🔹 Clinical Diagnosis (Primary)
No single confirmatory test.
🔹 Essential Features
✔ Chronic joint swelling or limitation
✔ Morning stiffness
✔ Pain improves with activity
✔ Reduced range of motion
🔬 Laboratory Findings (Supportive)
| Test | Significance |
|---|---|
| CBC | anemia, leukocytosis (systemic JIA) |
| ESR / CRP | inflammation |
| ANA | oligoarticular JIA, uveitis risk |
| RF | polyarticular RF+ |
| Anti-CCP | erosive disease predictor |
| Ferritin | very high in systemic JIA |
| HLA-B27 | ERA subtype |
🩻 Imaging
Early
- Ultrasound → synovitis, effusion
Later
- X-ray → joint space narrowing, erosions, growth abnormalities
- MRI → early synovitis & sacroiliitis
🚨 Important Diagnostic Exclusions
Before diagnosing JIA, rule out:
- Septic arthritis
- Tuberculosis
- Leukemia
- SLE
- Rheumatic fever
- Trauma
- Hemophilia
⚠️ Red Flags suggesting other diagnosis
- Severe bone pain at night → leukemia
- High fever with toxicity → infection
- Weight loss, pallor → malignancy
- Acute monoarthritis → septic arthritis
🧠 Exam Pearls (High Yield)
✔ Oligoarticular = most common
✔ Systemic JIA = quotidian fever + rash
✔ ANA+ girls → high uveitis risk
✔ RF+ polyarticular → resembles adult RA
✔ ERA → HLA-B27 boys, lower limb arthritis
✔ Screen for uveitis regularly even if asymptomatic